When it comes to birth control, women have a myriad of options to choose from. From birth control pills to condoms, the choices can be overwhelming. However, for those seeking a highly effective, long-lasting, and hassle-free contraceptive method, Mirena IUD might be the answer. In this comprehensive guide, we’ll explore everything you need to know about Mirena IUD, from its benefits and usage to potential side effects and frequently asked questions.
Related: 8 Best Ways To Avoid Pregnancy Naturally
What are the Different Types of IUDs available?
There are two types of IUDs available:
- Hormonal IUDs: Mirena, Kyleena, Liletta, and Skyla are hormonal IUDs that release the hormone progestin to prevent pregnancy. They are small, T-shaped plastic devices that are inserted into the uterus by a healthcare provider. Hormonal IUDs are effective for up to 3 to 8 years, depending on the type.
- Copper IUDs: Paragard is a non-hormonal IUD that is wrapped in a tiny bit of copper and can protect against pregnancy for up to 12 years. Copper IUDs work by creating an environment that is toxic to sperm, preventing fertilization.
What is Mirena IUD?
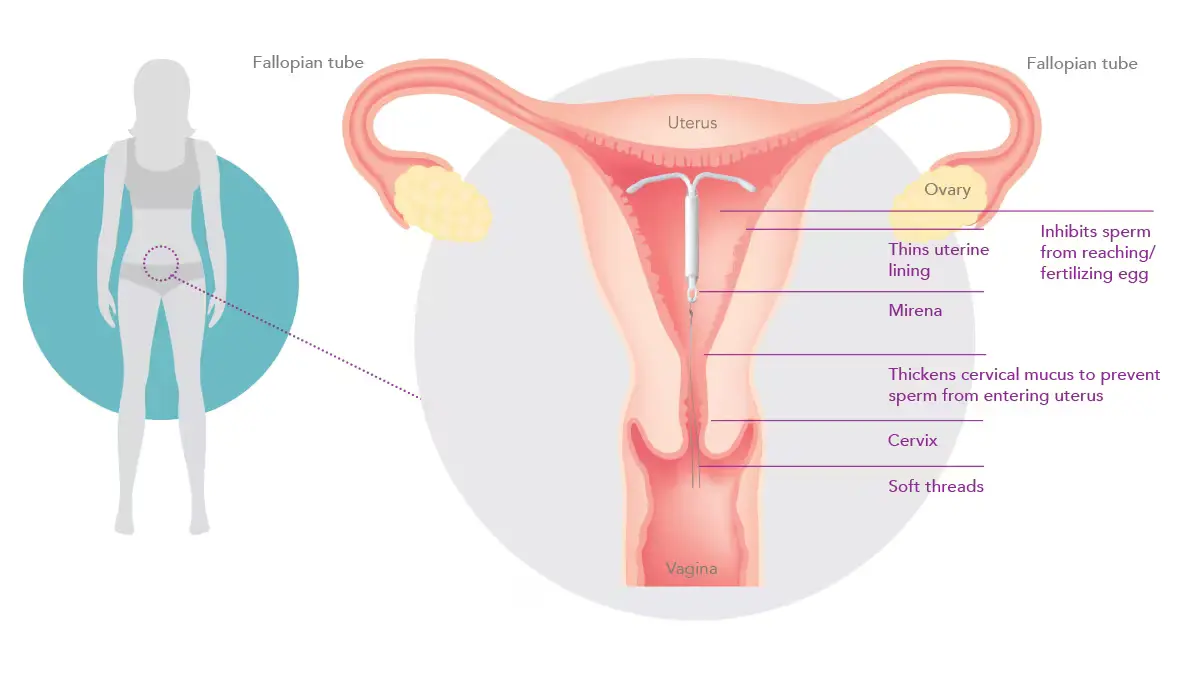
Mirena IUD is a small, T-shaped intrauterine device that’s inserted into the uterus to prevent pregnancy. It’s made of soft, flexible plastic and contains a hormone called levonorgestrel. It’s suitable whether or not you’ve had a baby. Mirena is highly effective, with over 99% effectiveness at preventing pregnancy for up to 8 years, resulting in less than 1 pregnancy per 100 women in a year. Additionally, it’s FDA-approved to treat heavy periods (heavy menstrual bleeding) for up to 5 years in women who choose an IUD for birth control.
Related: Marlissa Birth Control: An In-Depth Review of a Popular Contraceptive Option
How Mirena Works
How Does Mirena IUD Work?
Mirena IUD primarily works in three ways:
- Preventing Sperm Movement: The hormone levonorgestrel thickens the cervical mucus, making it difficult for sperm to move through the cervix and reach the egg.
- Inhibiting Egg Release: It also suppresses ovulation in some cases, preventing the release of eggs from the ovaries.
- Changing Uterine Lining: Mirena IUD changes the uterine lining, making it less receptive to a fertilized egg, thereby reducing the chance of pregnancy.
Does Mirena Start Working Right Away?
Mirena does not start working right away. It typically takes a few days to a week for Mirena to become effective in providing birth control once it has been inserted by a healthcare provider. During this initial period, it’s important to use an alternative form of contraception to prevent pregnancy until Mirena’s full contraceptive effect is established. If you have any concerns or questions about Mirena’s effectiveness, it’s advisable to consult with your healthcare provider for personalized guidance.
How Well Does Mirena Work?
Mirena is a highly effective form of birth control when used correctly. It is over 99% effective in preventing pregnancy, making it one of the most reliable contraceptive methods available. Its effectiveness is due to its long-lasting nature and the fact that it releases a low dose of the hormone levonorgestrel directly into the uterus, which helps prevent pregnancy by thickening cervical mucus and inhibiting sperm movement.
My Period After Mirena
Will My Periods Change Once I Get Mirena?
Mirena is an intrauterine device (IUD) that releases a low dose of a hormone called levonorgestrel. Many women experience changes in their menstrual bleeding patterns after getting Mirena. Some common changes include lighter periods, shorter periods, or even the absence of periods altogether. This is because Mirena can make the uterine lining thinner, which can lead to reduced menstrual bleeding. However, the specific changes in your periods can vary from person to person.
What If I Stop Getting My Period After I Get Mirena?
It is not uncommon for women to stop getting their periods while using Mirena. This is often considered a normal and expected side effect of the device. If you have concerns about not having periods while using Mirena, it’s a good idea to discuss them with your healthcare provider. They can help address any questions or concerns you may have.
Are There Any Other Side Effects or Risks with Mirena I Should Know About?
Mirena, like any medical intervention, can have side effects and risks. Some potential side effects of Mirena may include:
- Irregular bleeding or spotting, especially during the first few months after insertion.
- Pelvic pain or discomfort, particularly during the first few weeks after insertion.
- Headaches, breast tenderness, and mood changes.
There are also some less common but more serious risks associated with Mirena, such as:
- Perforation of the uterus during insertion.
- Infection, although this is rare.
- Ectopic pregnancy, although the risk is low.
It’s important to have a thorough discussion with your healthcare provider before getting Mirena to fully understand the potential risks and benefits in your individual case.
What If I Need Help with My Heavy Periods for More Than 5 Years?
If you continue to experience heavy periods or other menstrual issues after using Mirena for an extended period of time, it’s essential to consult with your healthcare provider. They can assess your specific situation, explore potential causes of your symptoms, and discuss alternative treatment options if necessary. There are various treatments available for managing heavy periods, and your healthcare provider can help determine the most appropriate approach for your long-term needs.
Pregnancy
Will I Be Able to Get Pregnant even though I have Mirena?
While Mirena is a highly effective form of contraception, there is still a small chance of pregnancy, although it’s relatively rare. If you are concerned about pregnancy or planning to conceive, it’s advisable to have your Mirena removed by a healthcare provider. Fertility typically returns soon after removal, but individual experiences may vary.
What If I want my Birth Control for More than 8 years?
Mirena is approved for contraceptive use for up to 8 years. If you are looking for long-term birth control beyond 8 years, you may need to discuss alternative contraceptive options with your healthcare provider. They can help you choose a method that aligns with your long-term family planning goals.
Can I try to get Pregnant as soon as Mirena is Removed?
Yes, you can try to conceive as soon as Mirena is removed. Unlike some other forms of contraception, Mirena does not have a prolonged effect on fertility after removal. In most cases, fertility returns quickly after the IUD is taken out. However, it’s essential to remember that the timing of conception can vary from person to person.
Can I Use Mirena While Breastfeeding?
Mirena can be used while breastfeeding, and it is often recommended as a suitable contraceptive option for breastfeeding mothers. The hormones in Mirena are primarily localized to the uterus and have minimal impact on breast milk production or the health of the breastfeeding infant. However, it’s a good idea to discuss your specific situation with a healthcare provider to ensure that Mirena is the right choice for you while breastfeeding.
How Soon Can I Get Mirena after having a Baby?
Mirena can be inserted shortly after childbirth, including immediately after delivery of the placenta or within the first 48 hours postpartum. This timing is often recommended because the cervix is more open during this period, making insertion easier. However, it’s important to discuss the timing of Mirena insertion with your healthcare provider, as individual circumstances and preferences may vary. They can help you determine the best timing for your specific situation.
Related: 10 Pregnancy Contraceptives
Mirena Placement
How is Mirena Placed?
Mirena is typically placed by a healthcare provider during a brief office visit. The procedure involves the following steps:
- You will lie on an examination table with your feet in stirrups, similar to a pelvic exam.
- The healthcare provider will insert a speculum into your vagina to visualize the cervix.
- The cervix is cleaned and may be numbed with a local anesthetic.
- Mirena is then inserted through the cervix and into the uterus.
- The strings attached to Mirena are trimmed to the appropriate length, and the device is positioned correctly.
- The healthcare provider will ensure that you are comfortable and may perform an ultrasound to verify the placement.
How Long Does it Take to Get Mirena?
Getting a Mirena IUD typically involves making an appointment with a healthcare provider, which can take a few days to a few weeks, depending on their availability. The actual placement procedure itself is relatively quick and usually takes only a few minutes.
What Does Placement Feel Like?
The experience of Mirena placement varies from person to person. Some individuals may experience mild discomfort or cramping during the procedure, while others may feel only a brief pinch or pressure. The cervix may be numbed to minimize discomfort. After the placement, some cramping and spotting can occur for a short period, but this usually subsides quickly.
How Should I Prepare for My Placement Appointment?
To prepare for your Mirena placement appointment, you can:
- Discuss any concerns or questions with your healthcare provider beforehand.
- Consider taking over-the-counter pain relievers (like ibuprofen) as advised by your healthcare provider to help with potential discomfort.
- Arrange for transportation to and from the appointment if you think you may feel uncomfortable afterward.
- Wear comfortable clothing.
Will I Be Able to go Back to Work/School After My Placement Appointment?
Most individuals are able to resume their normal activities, including work or school, shortly after the Mirena placement. However, you may experience some cramping and spotting for a few hours to a few days. It’s a good idea to have some pads or liners on hand, as well as pain relief medication if recommended by your healthcare provider, to help manage any discomfort. If you have concerns about how you will feel after the placement, you can discuss this with your healthcare provider during your appointment.
After placement
Will I Feel Mirena After it is Placed?
You may be aware of the presence of Mirena in your uterus shortly after it’s placed, but for most individuals, this sensation is temporary. Some people report mild cramping or a feeling of fullness in the lower abdomen for a few days to a week after insertion. However, over time, most individuals do not feel Mirena inside them.
How Will I Know that Mirena is Still in Place?
It’s essential to check periodically to ensure that Mirena is still in place. You can do this by feeling for the small strings attached to the IUD. The strings will extend down through the cervix into the upper part of your vagina. You can check for these strings by inserting a clean finger into your vagina. If you can feel the strings, Mirena is likely in its proper place. If you cannot feel the strings or feel something different, contact your healthcare provider, as this may indicate a potential issue with the IUD’s placement.
Can Mirena Fall Out?
While Mirena is designed to stay securely in place in the uterus, there is a rare chance that it can partially or fully expel from the uterus. This is more likely to occur shortly after insertion. If you experience severe pain, heavy bleeding, or if you cannot feel the strings or feel the IUD itself, contact your healthcare provider. They can assess the situation and determine whether the IUD needs to be repositioned or replaced.
How Often After Getting Mirena Should I come back to see You?
Typically, healthcare providers recommend a follow-up appointment a few weeks to a couple of months after Mirena insertion. During this follow-up appointment, your healthcare provider will check the placement of the IUD and address any concerns or questions you may have. After the initial follow-up, regular check-ups are usually scheduled on an annual basis. However, you should contact your healthcare provider if you experience any unusual symptoms, such as severe pain or heavy bleeding, between scheduled appointments. Additionally, it’s essential to follow your healthcare provider’s recommendations for when to have Mirena replaced, as it has a limited lifespan and will need to be removed and replaced after a certain number of years.
Can I Get Pregnant While Using Mirena IUD?
Yes, it is possible to get pregnant while using the Mirena intrauterine device (IUD), but the likelihood of pregnancy is very low. Mirena is one of the most effective forms of contraception available, with a failure rate of less than 1% in typical use.
Who Should Not Use Mirena IUD?

Mirena may not be your ideal match if:
- You’re expecting a bundle of joy – Mirena won’t work as a last-minute pregnancy stopper.
- You’ve wrestled with a severe pelvic infection known as pelvic inflammatory disease (PID), or you’ve had a bout of PID in the past – unless, of course, you’ve experienced a smooth pregnancy after the infection cleared.
- You’ve got an untreated genital infection brewing in your body.
- In the last three months, you’ve tangled with a serious pelvic infection following a pregnancy.
- You’re the magnet for infections, perhaps due to a bustling love life with multiple partners, immune system quirks, intravenous drug use, or other factors.
- Uterine or cervical cancer is on your radar, or you suspect it might be.
- Mysterious vaginal bleeding has you stumped.
- Your liver is giving you grief or hosting an unwelcome tumor.
- You’ve had a dance with breast cancer or any other progestin-sensitive cancer, be it recent or in the past.
- You’ve already got an intrauterine device cozying up in your uterus.
- Your uterus is going through some shape-shifting, thanks to the presence of hefty fibroid tumors.
- And last but not least, if you’re allergic to levonorgestrel, silicone, polyethylene, silica, barium sulfate, or iron oxide – Mirena might not be your best pal.
How Much Will Mirena Cost Me?
Here is the cost information for the Mirena IUD based on the search results:
- Cost with insurance: The cost of the Mirena IUD can vary depending on your insurance coverage. Some insurance plans may cover the full cost of the device, while others may require a copay or deductible. According to the Mirena website, eligible patients may be able to pay as little as $20 out of pocket for the device.
- Cost without insurance: Without insurance, the cost of the Mirena IUD can range from $500 to $1,300. The cost can vary depending on the healthcare provider and location. However, many Planned Parenthood health centers offer programs to make the IUD more affordable for people who don’t have or can’t use insurance.
- Additional costs: In addition to the cost of the device, there may be additional costs associated with getting the Mirena IUD inserted, such as the cost of the medical exam, insertion, and follow-up visits. According to the University of Michigan Health Services, the cost of Mirena insertion can range from $1,071 to $1,272, depending on the type of IUD.
How to Check If Your Insurance Will Cover Mirena?
- Dial the number on your insurance card’s back
- Inform them about Mirena, the healthcare provider-administered birth control
- Ask them to investigate if Mirena falls under the Affordable Care Act’s no-cost coverage umbrella
- Share the J code for Mirena: J7298, and the Current Procedural Terminology (CPT) code for Mirena placement: 58300
- Inquire about potential out-of-pocket expenses if Mirena isn’t fully covered by your plan
- Please take note: There might be other associated costs.
For comprehensive assistance in decoding your insurance coverage, explore CoverHer.org.”
Frequently Asked Questions (FAQs)
Is Mirena IUD painful to insert?
While some discomfort or cramping may occur during insertion, the procedure is generally well-tolerated and brief.
Can I still get pregnant after removing Mirena IUD?
Yes, your fertility returns quickly after removing the IUD, so you can conceive once it’s taken out.
Are there any age restrictions for using Mirena IUD?
Mirena IUD can be used by women of various ages, including those who have not given birth.
Does Mirena IUD protect against sexually transmitted infections (STIs)?
No, Mirena IUD is not a barrier against STIs. It only provides contraception.
What should I do if I suspect my Mirena IUD has been expelled?
Contact your healthcare provider immediately if you believe your IUD has been expelled.
Additional Resources
For more information about Mirena IUD and other contraceptive options, you can visit the following external links:
Download the Mirena Patient Brochure
If you’d like an additional reference for discussion with your healthcare provider, download this brochure and bring it with your questions to your next appointment.
Conclusion
In conclusion, Mirena IUD offers a convenient, highly effective, and long-lasting birth control option for women seeking to prevent pregnancy. It’s essential to consult with your healthcare provider to determine if Mirena IUD is suitable for your unique needs and to address any questions or concerns you may have. With proper care and follow-up, Mirena IUD can provide years of worry-free contraception.
Remember that while Mirena IUD is a reliable contraceptive, it does not protect against sexually transmitted infections, so it’s essential to practice safe sex when necessary.