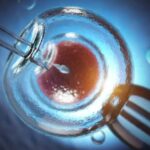
Ovulation is the process in a woman’s menstrual cycle in which an egg is released from the ovary. This typically occurs around day 14 of a 28-day cycle.
In fertility treatments like IUI (intrauterine insemination) and IVF (in vitro fertilization), ovulation is triggered through the use of hCG medication, known as a “trigger shot.” The timing of this trigger shot is critical, as it signals the body to ovulate within 24-48 hours. This allows the doctor to effectively time the sperm deposition or egg retrieval.
However, occasionally a woman’s body begins the ovulation process before the scheduled trigger shot. This is known as premature ovulation or early ovulation. When this happens, it can negatively impact the success rates of that fertility treatment cycle.
In this article, we will explore what early ovulation is, why it happens, how it’s detected, the impact it can have on IUI and IVF outcomes, how to prevent it, and next steps if it does occur. Understanding ovulation timing in fertility treatments is crucial for patients undergoing procedures like IUI and IVF.
Related: How Often Do I Need A Pap Smear?
What Happens If You Ovulate Before Trigger Shot?
If you ovulate before the trigger shot, it can impact the timing of fertility procedures. Ovulation typically occurs 24 to 36 hours after the trigger shot is administered. If the follicles have already ovulated before the trigger shot, there may be no eggs to be retrieved, affecting the success of the procedure. It’s important to follow the precise guidance of your doctor and administer the trigger shot at the recommended time to ensure the best possible outcome. Monitoring ovulation through ultrasound or blood tests is essential to confirm the timing of the trigger shot and optimize the chances of success.
Causes of Early Ovulation
Ovulation occurring earlier than expected before a trigger shot can happen for several reasons:
- Natural early ovulation – Some women naturally ovulate earlier in their cycle than expected. This can occur if you have a short follicular phase or your body gears up to ovulate sooner than the average 14 days after your period starts. Having a naturally early ovulation makes it more likely you’ll ovulate prematurely before the scheduled trigger shot.
- Miscalculated timing – Doctors determine the ideal timing for a trigger shot based on the size of your ovarian follicles. If follicles grow faster than expected or ovulation timing is misjudged, you may ovulate before the planned date. This is more likely if you have irregular cycles.
- Medication interactions – Certain fertility medications like clomiphene citrate can elevate estrogen and cause the body to ovulate sooner than normal. If you’re taking medications that affect hormones, it can inadvertently lead to early unexpected ovulation.
The trigger shot is carefully scheduled to time ovulation at the optimal point when fertilization is most likely. When ovulation happens earlier than planned, it can reduce the chances of successful conception in that cycle. Monitoring your body’s signals and communicating with your doctor can help avoid premature ovulation.
Monitoring Ovulation
There are a few different methods that can be used to monitor and detect ovulation each cycle:
Ovulation Prediction Kits (OPKs)
OPKs, also known as ovulation tests, detect the luteinizing hormone (LH) surge that happens 1-2 days before ovulation. They come in test strip form and work similarly to pregnancy tests – you either collect urine or dip the OPK in a cup of urine, and wait for colored lines to appear. There are two lines on the test – a control line and a test line. When the test line gets as dark or darker than the control line, this signals your LH surge. Once you detect this surge, you can expect to ovulate within the next 36 hours. OPKs are relatively inexpensive and easy to use.
Blood Tests
Your doctor can monitor certain hormones in the blood that fluctuate around ovulation. Estrogen rises in the days leading up to ovulation. LH and progesterone rise just before/around the time of ovulation. Your doctor may order blood tests to pinpoint the LH surge and confirm that ovulation took place afterwards based on progesterone levels. This is considered more accurate than OPKs but is more invasive and usually more expensive.
Ultrasounds
Pelvic ultrasounds performed by your doctor or fertility specialist allow them to actually visualize the development of ovarian follicles and the release of the egg. Ultrasounds can provide confirmation that ovulation is happening when intended based on the size of follicles and whether the follicle ruptures and collapses after ovulation. This is the most accurate way to confirm ovulation but also the most involved and expensive option.
Related: How to Prepare for Pregnancy After 40?
Impact on IUI Success
When ovulation occurs before the trigger shot, it can significantly reduce the chances of success for an IUI (intrauterine insemination) cycle. This is because timing is crucial for IUI. The sperm need to be in the fallopian tube at the time the egg is released in order for fertilization to occur.
If the egg is released from the ovary before insemination takes place, the chances that sperm and egg will meet are very low. Often, early ovulation results in cancellation of the IUI cycle altogether. Even if insemination happens, but later than intended, the chances of achieving pregnancy are diminished.
There are a couple reasons for the reduced chances of success:
- Lower Egg Quality – Eggs can only survive 12-24 hours after ovulation before they start to degrade. If the egg has already been released prior to insemination, it may be past its prime by the time sperm arrive. Older eggs have lower fertilization rates.
- Missed Timing – Sperm only survive 1-2 days inside the female reproductive tract. If the timing between ovulation and insemination is off even by 24 hours, the sperm may no longer be viable once the egg is released.
Proper timing is the key to IUI success. Unfortunately early ovulation throws off that timing, often to the point of cancelling the cycle altogether. Patients who experience premature ovulation should speak with their doctor about ways to prevent it in future cycles to maximize their chances of conception through IUI.
Impact on IVF Success
IVF treatment relies on precisely timed administration of fertility medications to stimulate the ovaries and synchronize egg development. If ovulation happens prematurely before egg retrieval, it can significantly lower the chances of IVF success. There are several key reasons for this:
- Lower number of eggs retrieved: The goal of ovarian stimulation is to develop multiple mature eggs during one stimulated cycle. Early ovulation results in loss of eggs that are ovulated before they can be collected. This leads to retrieval of fewer eggs, reducing the number available for fertilization.
- Reduced quality of embryos: In addition to lower egg numbers, the remaining embryos may be of poorer quality. The eggs ovulated early were not fully matured by medication stimulation. The eggs left behind may be more immature or abnormal. This further limits the number of high quality embryos.
- Lower implantation rates: With fewer embryos, and with potentially compromised embryo quality, a patient’s chance for successful implantation is reduced. Lower quality embryos have reduced viability and lower potential to implant and develop normally.
Overall, premature ovulation circumvents key steps in a timed and delicate IVF process. Loss of eggs and reduced embryo quality combine to lower one’s chances for a successful pregnancy. Proceeding with IVF despite early ovulation often leads to discouraging outcomes for patients. Consulting a physician and considering options to address ovulation issues can help improve chances for IVF success.
Related: When To Conceive To Have A Baby On New Year?
Preventing Early Ovulation
To prevent early ovulation during an IUI or IVF cycle, there are a few options your doctor may consider:
Start Stimulation Earlier
One way to prevent the follicles from maturing too fast is to start the ovarian stimulation medications a few days earlier in your cycle. By beginning the medications sooner, the goal is to slow down the follicle growth rate. This allows better control over the timing of maturation and ovulation.
Adjust Medication Dosage
If ovulation seems to be happening too early, your doctor may adjust the dosage of the medications being used for ovarian stimulation. Often, the dosage is lowered to help slow down follicle development. This helps delay ovulation until closer to the ideal timing.
Use GnRH Antagonists
GnRH antagonists are medications often used in IVF cycles to prevent premature ovulation. These medications work by blocking the body’s natural LH surge that causes ovulation. When a GnRH antagonist is added to the treatment protocol, it can help delay ovulation until the follicles are ready for egg retrieval. Using GnRH antagonists gives your doctor greater control over the ovulation timing.
By making changes such as starting medications sooner, adjusting dosages, or using GnRH antagonists, your doctor can help prevent follicles from maturing too quickly and ovulation from happening ahead of schedule. Careful monitoring and medication adjustments can optimize the timing for a successful IUI or IVF cycle.
Trigger Shot Timing
The trigger shot is a crucial part of the IVF process. Its timing can make all the difference in a successful outcome. The goal is to administer the trigger at the optimal time to maximize the chances of retrieving mature eggs. Here are some key points about trigger timing:
- The trigger shot causes the final maturation of the eggs and induces ovulation, so the eggs will be ready to be retrieved 34-36 hours later.
- The decision of when to give the trigger depends on the size and number of follicles. Typically, follicles should be ~18 mm before triggering.
- If given too early, the follicles may not be mature enough, increasing the risk of immature eggs at retrieval. If given too late, eggs may get overmature or ovulation could happen prematurely.
- Frequent monitoring in the final days of stimulation is key to pinpoint the perfect timing for trigger. The clinic will track follicle growth and estradiol levels.
- The trigger is usually given when there are at least 2-3 follicles measuring ≥17 mm. The largest follicle(s) should be around 20 mm.
- Women with PCOS may require larger follicle sizes (e.g. ≥21 mm) before trigger due to slower growth.
- HCG is the standard trigger medication. It mimics natural LH surge to induce final oocyte maturation and ovulation.
- Agonist triggers with Lupron are sometimes used to reduce risk of OHSS in high responders. This induces a shorter LH surge.
- Proper timing of the trigger shot is one of the most important factors for IVF success. Close monitoring and flexible protocols allow it to be precisely personalized.
Next Steps if Ovulation Occurs Early
If ovulation occurs before the trigger shot, you have a few options for next steps:
Cancel and Restart the Cycle
One option is to cancel the IUI or IVF cycle and restart with medications in the next cycle. This allows your body to reset and begin the controlled ovarian stimulation again when the time is right. Your doctor may recommend changing the medication protocol to better prevent early ovulation the next time.
Proceed with IUI/IVF
If ovulation happened just shortly before the scheduled IUI or egg retrieval, your doctor may recommend proceeding as planned. For IUI, sperm can live up to 5 days inside the body, so conception may still occur. With IVF, the eggs could be retrieved before they disintegrate if the timing is very close. However, chances of success decrease the further out ovulation occurs from the scheduled procedures.
Convert to Timed Intercourse
Another option is to switch the IUI or IVF cycle to timed intercourse. Have sex on the days leading up to and of ovulation to try conceiving naturally. This takes advantage of the follicle growth and timing from the medications. While not as effective as IUI or IVF, it offers a chance without canceling the cycle.
The best next step depends on your unique situation. Discuss the pros and cons of these options with your doctor. They can help determine the right path forward if ovulation happens too soon. The most important thing is not to get discouraged. There are still chances for pregnancy, and you can adjust for better timing on the next cycle.
Related: How Many Days After Sex Can You Take A Pregnancy Test?
Emotional Impact
Discovering that ovulation has occurred before the planned trigger shot can bring up many difficult feelings. There is often a sense of frustration and disappointment, as well as a feeling that a precious opportunity was lost.
Many women describe feeling angry with their bodies for not cooperating with the carefully timed fertility treatment schedule. There can also be sadness and grief over the missed chance to conceive that cycle. Some women may feel guilt or blame themselves, even though early ovulation is not their fault.
Going through fertility treatments is already an emotional rollercoaster. When ovulation happens early, it can make women feel even more out of control and heighten anxiety. There may be fears that it will happen again or concerns about being able to get pregnant.
It’s important to acknowledge these feelings of frustration, disappointment and lost opportunity. Having empathy for yourself in this challenging situation can help ease the emotional impact. Discussing your experience with your partner, doctor and support system can also help provide some relief.
While early ovulation can be disheartening, it’s important to remember it’s no one’s fault. With an understanding medical team and your own self-compassion, you can get through this hurdle on the road to building your family.
Conclusion
Ovulating before the trigger shot can be disappointing and frustrating, but it’s important not to lose hope. With close monitoring and proper timing, success is still possible in future cycles.
This article summarized the causes, impacts, and prevention of early ovulation. The key points are:
- Careful monitoring is essential to pinpoint ovulation and administer the trigger at the right time. This involves ultrasounds to check follicle growth and blood tests to detect the LH surge.
- If ovulation happens before the trigger shot, IUI and IVF success rates are lower that cycle. However, early ovulation doesn’t mean you can’t get pregnant. Sperm can sometimes still fertilize the egg.
- If it occurs repeatedly, early ovulation may indicate an underlying hormone imbalance. Your doctor can provide medication to better control the ovulation timing.
- While emotionally difficult, remember one unsuccessful cycle does not define your fertility journey. With your doctor’s guidance, continue optimizing the timing and protocol. Control what you can, and trust your body will cooperate in its own time.
Stay hopeful and don’t give up. With perseverance and the right medical care, you can still achieve your dream of having a baby. Each cycle provides more information to bring you closer to success.
Related: Will Ovulation Test Be Positive If Pregnant?
Frequently Asked Questions (FAQs)
What happens if you ovulate before the trigger shot IUI?
If I surge, should I still take the trigger shot?
If you experience a natural surge, it’s important to consult your healthcare provider. They will advise whether or not to proceed with the trigger shot. In some cases, a natural surge may eliminate the need for the trigger shot, but this decision should be made in consultation with a medical professional.
What happens if you take the trigger shot late?
Does a trigger shot guarantee ovulation?
Can you ovulate 12 hours after the trigger shot?
Ovulation typically occurs 24-36 hours after the trigger shot. While it’s less common to ovulate as early as 12 hours after the shot, the timing of ovulation can vary among individuals. It’s important to follow the guidance of your healthcare provider regarding the timing of intercourse or other fertility procedures after the trigger shot.
What Are The Symptoms of ovulation after the HCG injection?
Symptoms of ovulation after the HCG injection can include mild abdominal pain, bloating, and a change in cervical mucus. However, not everyone experiences noticeable symptoms of ovulation. Monitoring ovulation through ultrasound or blood tests is a more accurate way to confirm ovulation after the HCG injection.