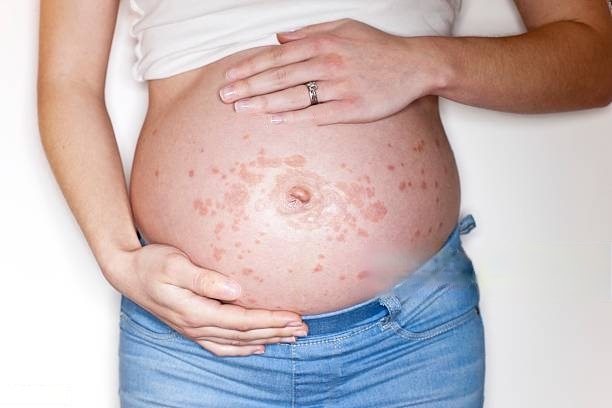
Pregnancy is a phase of life that can cause several skin changes and rashes. These skin changes are very common and are not to be of concern. These normal skin changes should not be mistaken for a rash. The normal skin changes in pregnancy are melasma or chloasma, darkening of preexisting moles, linea nigra, stria gravidarum and acne. Pregnancy rash is different from all these regular changes and sometimes might need medical help. If you’re experiencing a pregnancy rash or skin itching, it’s normal, and several factors can be the reason behind it.
The reasons behind pregnancy rash can range from minor issues such as heat rash to more serious underlying medical problems, like liver or thyroid disease. Some women may already have pre-existing conditions such as eczema, which can lead to a pregnancy rash, while others may develop new skin changes for the first time.
This article aims to shed light on some of the reasons why you might experience a new rash on your face or belly during pregnancy. It also offers practical tips and ideas for relieving the discomfort caused by these rashes.
Related: Best 10 Pregnancy Pillows for Happy Pregnancy
Are Pregnancy Rashes an Indication of Early Pregnancy?
It is commonly believed that skin rashes can be an early sign of pregnancy. However, this is a misconception as skin rashes are not considered to be a reliable indicator of early pregnancy. In most cases, rashes tend to appear during the later stages of pregnancy.
If you suspect you might be pregnant, it is essential to look for other symptoms that can confirm your doubts. Some of the most common signs of early pregnancy include frequent urination, breast tenderness, nausea or vomiting, fatigue, and a missed period.
While skin rashes may not be an early sign of pregnancy, hormonal shifts during pregnancy can cause various changes in the body, including skin-related issues. Hence, if you notice a new rash or any other unusual changes, it may be related to pregnancy. In such cases, it is advisable to take a home pregnancy test or visit a doctor to confirm your pregnancy.
Related: 10 Best Pregnancy Support Belts: Supporting Your Belly and Back
7 Types of Skin Rashes and Changes that can occur During Pregnancy
During pregnancy, a woman’s body undergoes a complex series of changes that impact almost every organ and process, including the skin. Unfortunately, one of the potential consequences of these changes is the development of rashes. These rashes are quite common, affecting between 18% and 40% of pregnant women, and are considered chronic if they persist for more than six weeks.
Fortunately, most pregnancy-related rashes are not serious and do not pose any risk to the developing fetus. This is the case with rashes caused by pregnancy-related conditions such as:
- Atopic Eruption of Pregnancy (AEP), a collection of common pregnancy rashes
- Polymorphic Eruption of Pregnancy (PEP), which used to be known as PUPPP
- Pemphigoid Gestationis
- Impetigo Herpetiformis, also called Pustular Psoriasis of Pregnancy (PPP).
However, in some instances, a rash during pregnancy can be a sign of a more severe, pregnancy-related condition such as cholestasis of pregnancy. This condition impacts the liver and can be a significant threat to both the mother’s health and the baby’s. Home remedies are not appropriate for managing this condition, and it is important to consult with a healthcare provider.
It is essential to remember that other factors, such as gestational diabetes, can contribute to skin rashes and itching. Additionally, skin issues unrelated to pregnancy, such as psoriasis or contact dermatitis, can also cause rashes during pregnancy.
Related: The 16 Best Tweens Bra for Training in 2023
Atopic Eruption of Pregnancy
During pregnancy, women’s bodies undergo several changes, including hormonal imbalances that can cause skin rashes. Atopic eruption of pregnancy (AEP) is a group of pregnancy rashes that include several types, each with its unique characteristics.
“Atopic” refers to the body’s tendency to produce antibodies in response to a trigger due to an underlying genetic factor. This is similar to atopic eczema, which accounts for about 50% of all pregnancy-related skin conditions.
AEP typically occurs before the third trimester, and women with pre-existing skin conditions like eczema are at a higher risk of developing it. In fact, about 20% of AEP cases occur in women who already have eczema and experience a flare-up of symptoms during pregnancy.
Atopic Eczema
Atopic Eczema is the most common type of AEP. It usually affects women who are pregnant for the first time, but those with a family history of related conditions such as asthma or hay fever allergies are also at risk. Symptoms of atopic eczema include itchy, dry, and red patches of skin, primarily on the neck or breasts. Creams and moisturizers can be used to treat it, but sometimes, steroid creams and antihistamines are necessary.
Prurigo of Pregnancy (PP)
Prurigo of pregnancy (PP) is another type of AEP that may emerge for the first time during pregnancy, usually in the latter half. It is characterized by itchy, raised bumps on the arms, legs, and occasionally the abdomen, which often cluster together in groups. PP is treated with moisturizers, topical steroids, and oral antihistamines. Although the rash usually resolves shortly after delivery, it may recur in future pregnancies.
Pruritic Folliculitis of Pregnancy (PFP)
Pruritic Folliculitis of Pregnancy (PFP) is a rare type of pregnancy rash that affects about 1 in 3,000 pregnancies during the second and third trimesters. It causes an itchy, red rash that looks like acne on the chest, arms, shoulders, and back. There is no clear link to an underlying history of allergic or skin conditions, and the rash usually goes away within a month or two after delivery. Treatment includes topical acne treatments such as benzoyl peroxide, topical steroids, and oral antihistamines.
Polymorphic Eruption of Pregnancy (PEP) or PUPPP
Polymorphic Eruption of Pregnancy (PEP), also referred to as pruritic urticarial papules and plaques of pregnancy (PUPPP), is a skin condition that affects expecting mothers. It usually appears in the third trimester or after delivery in the first pregnancy and affects around 1 in 160 pregnancies.
PUPPP causes a rash that is extremely itchy and looks similar to an allergic skin rash or hives. The rash mostly appears on the abdomen and is likely to be a result of the stretching of the skin.
The treatment of PUPPP generally involves the use of oral antihistamines and topical steroids. In some cases, oral steroids may also be necessary to alleviate the symptoms.
If you suspect that you have PUPPP, it is important to speak to your healthcare provider for proper diagnosis and treatment.
Related: PUPPP Rash: Symptoms, Causes, Treatments and Prevention
Pemphigoid Gestationis
Pemphigoid gestationis (PG), formerly known as herpes gestationis, is a pregnancy-related autoimmune condition that affects approximately 1 in 50,000 pregnancies. Although it is called herpes gestationis, it is not caused by a herpes virus infection. This condition may produce a rash similar in appearance to herpes, with fluid-filled bumps and blisters on the abdomen, especially around the belly button, and an overall skin rash that forms in ring patterns.
PG typically occurs during the second or third trimester of pregnancy, and if you have had it in the past, it is likely to recur in future pregnancies. Treatment usually involves the use of topical or oral corticosteroids.
Previously, PG was considered relatively harmless to the developing fetus, although it was associated with premature delivery. However, recent studies have shown that PG may also lead to fetal growth restriction (FGR), where the baby is in the lowest 10% in terms of birth weight for the given stage of pregnancy. FGR indicates that the placenta is unable to provide the necessary nourishment and oxygen for the fetus, which greatly increases the risk of stillbirth or neonatal complications.
Additionally, 10% of newborns may experience PG-related neonatal pemphigoid, which means the baby also develops a skin condition with hives and skin-layer changes. Although this condition heals, it adds further complexity to the pregnancy and delivery.
Impetigo Herpetiformis
Impetigo herpetiformis is a rare form of psoriasis that is associated with pregnancy and can be life-threatening. It typically develops during the third trimester and disappears after delivery. Although the precise cause of this condition remains unclear, there is some evidence suggesting that genetics may be a factor, and it may recur in subsequent pregnancies.
This condition is characterized by clusters of red, crusty lesions on the skin. However, it can also cause systemic symptoms, such as nausea, vomiting, fever, chills, seizures, and hypovolemic shock. It can also affect fetal development, potentially leading to premature birth, oxygen and nutrient deficiencies through the placenta, and stillbirth, which are similar to the effects of PG.
Individuals with impetigo herpetiformis often have low levels of calcium, but the underlying reasons for this are not yet fully understood. While antibiotics are typically prescribed to treat this condition, more severe cases may require a range of interventions.
Cholestasis of Pregnancy
This condition usually presents itself in the third trimester and is caused by a buildup of bile acids in the bloodstream from the gallbladder and biliary system.
One of the most common symptoms of cholestasis of pregnancy is itching, which can be intense and persistent. While there is no rash associated with the condition, it may cause skin jaundice, a yellowing of the skin. Fortunately, the itching usually subsides after delivery, but there is a possibility that it may reoccur in subsequent pregnancies.
It’s essential to note that cholestasis of pregnancy can have adverse effects on the fetus. The buildup of bile acids can lead to fetal distress due to a lack of oxygen, which can result in premature birth. Fortunately, there are treatment options available to manage the condition.
Hives
Hives, also known as urticaria, are a skin condition characterized by raised bumps that can appear alone or in clusters of red spots or patches. These bumps can appear anywhere on the body and often cause an intense itching sensation. In some cases, they may even feel like they are burning or stinging.
Hives can occur suddenly and disappear just as quickly, usually within a few days to six weeks. They are typically caused by the release of histamine in response to various stimuli such as emotional stress, hormonal changes, or infections. In some cases, they may be a sign of an allergic reaction to food, insect bites, pollen, or other triggers.
If you are experiencing hives, it is essential to rule out an allergic reaction, particularly if you have other symptoms of anaphylaxis, which can be life-threatening. Symptoms of anaphylaxis include a rapid pulse, swollen tongue, tingling in your hands, feet, or scalp, and difficulty breathing.
The treatment for hives may involve taking antihistamines or corticosteroids to help reduce inflammation. However, if you are experiencing signs of anaphylaxis, it is crucial to seek emergency medical attention immediately.
Heat Rash
Heat rash, also known as prickly heat, is a common skin condition caused by excessive sweating that can occur anywhere on the body. When you are pregnant, your body temperature increases, which makes you more susceptible to heat rash during this period.
Heat rash is characterized by an itchy or prickly sensation accompanied by small spots, redness, and sometimes even swelling. You can identify this type of rash using pictures for reference. Fortunately, this rash usually resolves on its own within a few days and does not pose any risk to your baby.
While heat rash does not necessarily require specific treatment, there are some things you can do to alleviate the symptoms. You may want to consider using antihistamines or calamine lotion to soothe the itchiness. Additionally, staying cool and avoiding activities that lead to sweating can be very helpful.
Related: 6 Safe Pregnancy Exercises For Normal Delivery
Natural Remedies for Pregnancy Rashes
One of the most common ways to alleviate the discomfort caused by pregnancy rashes is to use moisturizers or over-the-counter medications. Additionally, it’s recommended to wear loose-fitting clothing and take soothing baths. However, it’s important to avoid products that may dry out your skin, as this can exacerbate the condition.
If you’re using creams for stretch marks, try massaging them into your skin for more effective results, according to a recent study. In case of AEP and PEP conditions, start by using creams and moisturizers. If they don’t bring relief, you can then consider using steroid creams or antihistamine drugs. However, it’s always best to consult your healthcare provider before using prescription drugs or UVB light treatments.
It’s important to keep in mind that the treatment for pregnancy rashes may differ depending on the trimester you’re in, as well as the potential effects of medications on your fetus. For instance, UVB light treatments are generally safer in early pregnancy than many prescription drugs.
Related: 7 Best Home Remedies to Cure Itching During Pregnancy
Natural Home Remedies To Ease Itching During Pregnancy
Some of the medical conditions such as cholestasis, pruritic urticarial papules And plaques of pregnancy (PUPP), and prurigo can cause itchiness. Fortunately, there are many natural remedies available that can help alleviate this problem. Here are some effective remedies that can soothe and calm irritated skin.
Oatmeal
Oatmeal has natural anti-inflammatory and antipruritic properties that make it an excellent remedy for dealing with itchy and inflamed skin. A powerful antioxidant compound found in oats called Aventhramides is responsible for soothing itchy and irritated skin. Oatmeal-based products can revamp your skin health in amazing ways.
How to use: Add one cup of oatmeal to a tub filled with water and soak in it for 20 minutes. Repeat this process once daily to get relief from itchiness.
Coconut Oil
Coconut oil contains lauric acid which works as an effective anti-inflammatory agent that can help calm itchy skin. Additionally, coconut oil is a natural moisturizer and can work wonders in healing common skin issues like dry skin, psoriasis, and eczema. Virgin coconut oil has many uses, nutrition, and health benefits that can be beneficial for skin health.
How to Use
Take some coconut oil in your palm, rub it well and gently massage it onto the affected regions. Allow it to soak for 30-40 minutes or leave it on overnight before rinsing it off. Repeat this process once daily to soothe itchy and irritated skin.
Aloe Vera Gel
Aloe vera is a time-tested remedy for treating various skin problems and infections. It contains phyto-components that exhibit anti-inflammatory, soothing, and cooling properties that can reduce itching and dry skin.
How to Use
Gently massage aloe vera gel onto the affected regions, leave it on for 30 minutes and rinse off with water. Repeat this process 2-3 times a week for the best result.
Essential Oils
Essential oils such as rose geranium and juniper oil have strong anti-itch and anti-inflammatory properties that make them valuable in treating itchy skin. These oils can also help reduce inflammation and swelling.
How to Use
In a mixing bowl, add about 10-12 drops of any essential oil and blend it with 2 tbsp. of carrier oil like coconut. Apply it to the affected regions and leave it on for an hour before rinsing it off. Repeat this process twice daily to alleviate itchiness.
Lemon Juice
Lemon juice has a soothing property that can be useful in lessening itchy skin issues. It is also a good antimicrobial agent that can help ward off germs present on the surface of the skin. Furthermore, the acidic nature of lemon juice helps in balancing the pH of the skin, thereby reducing skin inflammation.
How to Use
Mix one tablespoon of lemon juice well with a quarter cup of water, dab a cotton pad in this solution, and apply it to the affected regions. Leave it on for 30 minutes before rinsing it off.
Chickpea Flour
Chickpea flour is an excellent natural remedy for treating all kinds of skin and beauty woes. This humble kitchen ingredient works amazingly well in providing instant relief from skin irritation, inflammation, and itchiness.
How to Use
Mix one tablespoon of gram flour with curd to form a fine paste. Apply it to the affected regions, let it dry, and then wash off after 30 minutes. Try this once daily for the best results.
When to See a Doctor?
It’s a good idea to talk to your healthcare provider about any product you use to relieve the symptoms of a pregnancy rash. It also will be necessary if you have an AEP or PEP condition that doesn’t respond to treatments at home. With pemphigoid gestationis, impetigo herpetiformis, and cholestasis of pregnancy, you’ll need professional care to ensure that both you and your baby are healthy and safe. Since it’s hard to know what type of pregnancy rash you have on your own, let your obstetrician or midwife know about it even if you are getting relief from simple home remedies.
How Your Doctor will Diagnose Your Rash?
When you visit your doctor for a pregnancy rash, they will conduct a thorough examination and inquire about the onset, spread, and duration of your symptoms. To determine the underlying cause, they will also inquire about any other accompanying symptoms.
Depending on the type of rash, your doctor may order additional tests. For instance, a blood test can check for signs of infection or bile levels. In the case of rashes caused by triggers such as hives, allergy tests involving skin or blood samples may be useful. A skin biopsy may also be necessary to allow your doctor to examine the rash under a microscope.
Certain conditions such as cholestasis may have a genetic component or be linked to a history of liver disease or pregnancy with multiples. Therefore, it’s essential to mention any relevant information from your personal or family medical history that might aid in diagnosis, even if it seems insignificant.
Related: Pregnancy Tips And Ideas To Make The Road Smoother
Is Pregnancy Rash Dangerous?
Pregnancy rash is usually not dangerous, but it can be uncomfortable and sometimes painful. If you experience severe itching or notice any signs of infection, such as pus or red streaks, you should contact your healthcare provider.
Can Pregnancy Rash be Prevented?
While pregnancy rash cannot always be prevented, there are some steps you can take to reduce your risk of developing it. These include keeping your skin cool and dry, using gentle cleansers and moisturizers, and avoiding harsh chemicals and fragrances.
Can I Use Over-the-Counter Creams for Pregnancy Rash?
Some over-the-counter creams may be safe to use for pregnancy rash, but it’s important to check with your healthcare provider before using any new products. They can help you determine which products are safe and effective for you to use during pregnancy.












